Medicare
Protecting affordability in a pandemic — Experts find fair prices for remdesivir between $10 and $4,500
In a nation hungry for good news in fighting the COVID-19 pandemic, remdesivir has emerged as a first ray of hope. The FDA has quickly approved the drug for emergency use with seriously ill patients. However there are concerns that the data supporting remdesivir’s effectiveness has not been published or peer reviewed by independent scientists…
Read MoreCongressional move to rein in innovations that harm people, Connecticut advocates’ SIM concerns addressed in DC
A new bill in Congress, proposed by both Democrats and Republicans, would place controls on federal grants for payment and delivery reform projects. The Strengthening Innovation in Medicare and Medicaid Act was introduced last week to “increase transparency and accountability within the federal Center for Medicare and Medicaid Innovation (CMMI)”. CMMI is the federal agency…
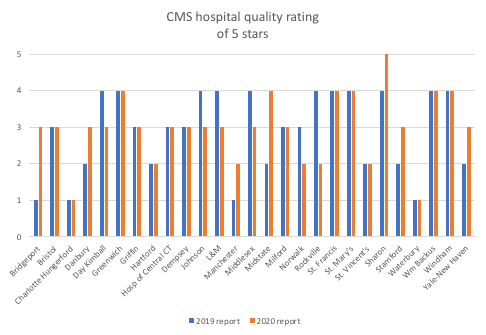
Read MoreCT hospital quality still lacking
New Medicare hospital quality ratings find little change from last year’s report. Almost half of Connecticut hospitals received three stars out of five, about the same as last year. Quality ratings didn’t change for half of Connecticut hospitals. This confirms a long history of underperformance by Connecticut hospitals. We did have one five-star hospital (Sharon)…
Read MorePCMH (no Plus) program continues to grow and improve care
At MAPOC’s Care Management Committee meeting Wednesday, the state provided the latest numbers from the successful Person-Centered Medical Home program. PCMHs are primary care practices that coordinate care for patients, offer expanded hours, and address population health needs. The program continues to grow, adding 52 primary care providers and seven new sites of care in…
Read MoreSurvey finds CT ACOs planning services for high need members
Similar to national results, a new survey of Connecticut Accountable Care Organizations for MAPOC’s Complex Care Committee by the CT Health Policy Project finds that most are using multiple methods to identify high need members. But they are still working on implementing effective programs to address the needs. Many of their plans follow best practices…
Read MoreICER seeks input on non-drug topics for 2020
The Institute for Clinical and Economic Review is seeking input on non-drug topics they should study for 2020. An independent nonprofit research institute, ICER is the US leader in assessing the evidence on the effectiveness and value of drugs and other medical services. ICER’s reports and pricing benchmarks that represent a good value for consumers…
Read MoreBipartisan Insurance Committee forum finds a lot of consensus on potential reforms
Download the CTHPP presentation Yesterday the Chairs and Ranking Members of the Insurance Committee convened a forum on potential reforms to lower healthcare costs. Legislators invited David Seltz from the Massachusetts Health Policy Commission. Connecticut speakers included representatives from the insurance industry, providers, state officials, a foundation and advocates. A recurring theme was the need…
Read MoreConnecticut’s uninsured rate stabilizes, retaining ACA gains
Download the report New numbers from the US Census Bureau report that 187,000 or 5.3% of Connecticut residents were uninsured last year. That number is down slightly from the year before when the uninsured rate was 5.5%, but above 2016’s rate at 4.9%. The new data continues the trend of fewer uninsured that began with…
Read MoreCoincidence? CT spends little on primary care, and we have high ED, preventable hospitalization rates
A new analysis finds that Connecticut, at only 3.5% of our health care dollars spent on primary care, is last among 29 states studied. Not surprisingly, we also rank among the highest in ED visits, all hospitalizations, and in avoidable hospitalizations. The US average is 5.6% of health care spending devoted to primary care, well…
Read MoreLarge study finds selection bias in Medicare shared savings erases savings and quality improvements – advocates saw this coming
Researchers from the University of Michigan found that the modest savings and quality improvements reported by Medicare’s extensive shared savings program (MSSP) are likely due to adverse selection. High cost clinicians and beneficiaries were far more likely than others to exit the program. When adjusted for the selective bias in MSSP exit, reported savings and…
Read More