PCCM
Cost Cap primary care project only focusing on raising spending, not services
At the October 26th Primary Care Subgroup meeting, in response to questioning by a member, the Office of Health Strategy’s (OHS) consultants repeatedly confirmed that the goal of the Cost Cap provision on primary care is solely to raise spending, not to increase services. Members raised serious concerns about sending more money into the current…
Read MoreSign on letter voices deep concerns with primary care capitation
Today twenty-five independent advocates and providers signed a letter to the Office of Health Strategy opposing capitation of primary care services across Connecticut. The letter shares serious concerns with the Office of Health Strategy’s (OHS) plan to shift all primary care in Connecticut to a capitated payment model. The current concerns echo advocates’ and legislators’…
Read MoreCTNJ op-ed: Patient-centered or doctor-centered? Primary care planning is off track
Several state agencies and their committees are planning to expand primary care in Connecticut – that’s a good thing. But it’s being driven by primary care doctors and their needs rather than patients. Read more
Read MoreGood and bad Medicaid PCMH, PCMH Plus updates
At today’s MAPOC Care Management Committee, we learned that Medicaid’s successful Patient-Centered Medical Home (PCMH) program is growing and keeping up with higher enrollment due to COVID. In disappointing news, we also learned that the controversial PCMH Plus program has fewer care managers than expected and only 36% of ACO member advisory committees have any…
Read MoreOHS committee considering dumbing down successful PCMH standards
Among other troubling plans, the Office of Health Strategy’s Primary Care Subgroup is considering four options to certify high-performing primary care practices for higher levels of reimbursement. The committee is deciding how to double spending on primary care while simultaneously capping healthcare cost growth. At their meeting this week, the committee of mainly primary care…
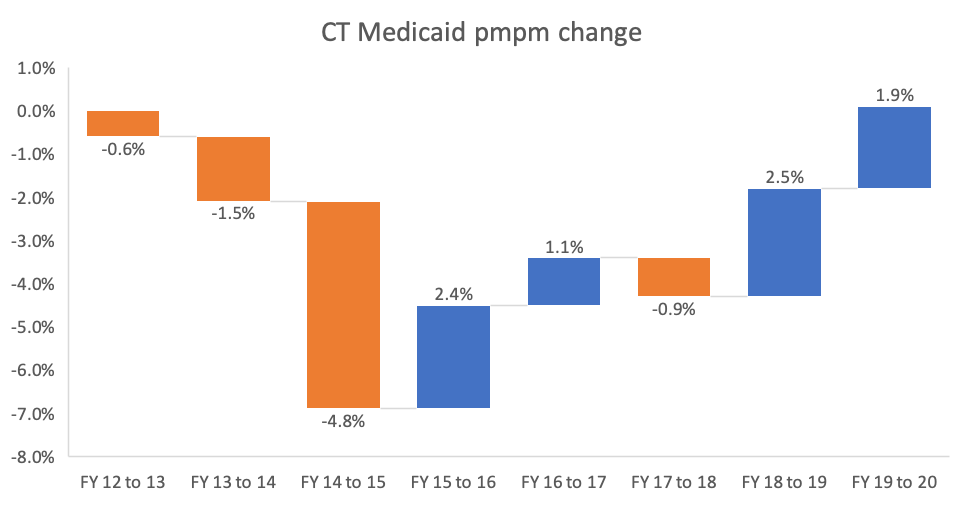
Read MoreConnecticut Medicaid costs stable but rising physician and clinic spending threaten progress
Download the report Since switching from managed care organizations in 2012 to focus on care management, Connecticut Medicaid spending has stabilized while enrollment has expanded significantly, according to the state’s latest financial report. Medicaid now covers one in four state residents. However, physician and clinic spending increases are eroding early progress in controlling costs. Medicaid…
Read MoreTop Stories of 2020
A year ago, our predictions for 2020 missed all but the recession. COVID has us giving up on predictions, so we’ll just take a look back at our top stories of this year. Advocacy Toolbox now online — Updates include specific, real world tools for legislative, administrative, and state budget advocacy, how to change public…
Read MoreCTNJ Op-Ed: Labels matter in healthcare, especially the misleading ones
The President was right – healthcare is complicated. There are lots of reasons, but a big one is language. What something is called can add to or lessen understanding. Sometimes it can be deceptive, giving the impression of a more acceptable definition than the truth. It rarely works for long, but a lot of harm…
Read MoreCOVID hit Medicaid hard
Medicaid members were about 33% more likely to be diagnosed with COVID than other Connecticut residents, according to CHNCT’s presentation Friday to the Medicaid oversight council. The average age of members with COVID was 52 years but ranged from newborn to 102 years old. Like the rest of the population, COVID hit Medicaid members with…
Read MoreSurprisingly, Medicaid applications are down sharply with the pandemic
At Friday’s MAPOC meeting, DSS reported that HUSKY applications were down 40% in May from a year before. This was unexpected given massive increases in unemployment and predictions of over 100,000 new Connecticut Medicaid members because of the pandemic. In January, February and March, applications ran 15% to 20% higher than last year. But a…
Read More