Anthem keeps lion’s share of CT insurance market
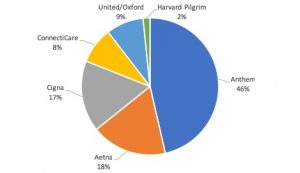 The best-kept secret in CT healthcare – the Insurance Department’s Consumer Report Card on Managed Care Plans – is out again this year covering 2017. Once again, Anthem has the lion’s share of the market at 46%. ConnectiCare lost almost 55,000 members between 2016 and 2017. About two out of three insured people in Connecticut are in fully insured plans. The majority are in large group plans (83%), 11% are in small groups and 6% of us are buying individual coverage. Medical loss ratios, the percent of premiums insurers spend on medical care, are comfortably over 85%, except Aetna’s large group and individual plans. Detailed care quality scores include follow up after mental health hospitalization, after ER visits for drug and alcohol dependence, controlling high blood pressure, and cancer screenings. Per member per month spending by category by plan and participating providers by county are fascinating. The report includes more detail on enrollment, tons of information on reasons that claims were denied and utilization reviews, consumer satisfaction levels, quality ratings of plans, helpful contact information for consumers to reach their plan and a glossary of all those unintelligible insurance terms.
The best-kept secret in CT healthcare – the Insurance Department’s Consumer Report Card on Managed Care Plans – is out again this year covering 2017. Once again, Anthem has the lion’s share of the market at 46%. ConnectiCare lost almost 55,000 members between 2016 and 2017. About two out of three insured people in Connecticut are in fully insured plans. The majority are in large group plans (83%), 11% are in small groups and 6% of us are buying individual coverage. Medical loss ratios, the percent of premiums insurers spend on medical care, are comfortably over 85%, except Aetna’s large group and individual plans. Detailed care quality scores include follow up after mental health hospitalization, after ER visits for drug and alcohol dependence, controlling high blood pressure, and cancer screenings. Per member per month spending by category by plan and participating providers by county are fascinating. The report includes more detail on enrollment, tons of information on reasons that claims were denied and utilization reviews, consumer satisfaction levels, quality ratings of plans, helpful contact information for consumers to reach their plan and a glossary of all those unintelligible insurance terms.

